This blog was written by Shaheena Salim Jumani-Alwani, MPhil scholar at Aga Khan University Institute for Educational Development. Shaheena has more than 20 years of experience as a Nurse Leader, and is alumna of Aga Khan University School of Nursing and Midwifery and the University of the West of Scotland.
This blog explores the intricate relationship between mental wellbeing and academic performance among undergraduate nursing students at a tertiary care hospital in Karachi, Pakistan. This study captures the lived experiences of 24 students, offering insights into mental health challenges that influence their academic performances. The findings highlight the need for institutional support, emotional literacy and policy integration within nursing curricula.
Mental health and academic performance are intricately connected. Students recognise how academic stress, emotion regulation, stigma and the role of institutional support influence their academic success. This study is grounded in a constructivist approach, valuing co-constructed realities, emphasising participants’ voices and ethical engagement. The study asks how undergraduate nursing students perceive the relationship between their mental wellbeing and academic performance.
Academic pressure
The most recurrent theme was academic overload, with participants expressing that the intensity of assessments, clinical requirements and emotional labour of caregiving were mentally taxing. Students repeatedly associated heavy academic loads with symptoms of anxiety, fatigue, sleep disturbances, reduced appetite and in some cases, visiting psychologists. Few mentioned that despite their passion for nursing, the relentless academic expectations undermined their sense of self-efficacy. Such academic load, particularly when combined with caring for critically-ill patients, intensified psychological strain.
Institutional support
Participants discussed the lack of institutional mechanisms to support mental wellbeing. Some recounted instances, when mental distress was dismissed or misunderstood by faculty. Others described a sense of relief when individual teachers showed compassion or extended deadlines, indicating how even minor institutional accommodations could buffer stress.
Stigma
Stigma surrounding mental health was prominent. Despite knowing about counselling services, most participants avoided using them due to fear of being labelled as ‘unstable’ or ‘unfit for nursing’. Students preferred to share with trusted friends and rely on self-help strategies, like meditation and prayers.
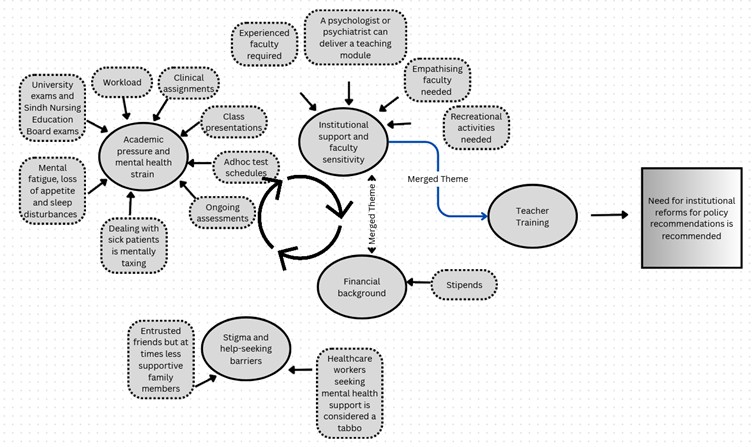
Emerging themes have been summarised in Figure 1. This illustrates the complex interplay between academic pressures, institutional support systems, financial challenges and stigma surrounding mental health. Overarching issues such as ad-hoc test schedules and emotionally-demanding clinical environments are central to the student experience.
The diagram also indicates actionable areas, such as teacher training, faculty sensitivity and institutional reform (as potential leverage points for systemic improvement). These insights can inform evidence-based educational policies that support student resilience and mental health literacy within nursing education.
This study affirms the critical connection between mental health and academic performance in nursing students. Despite high academic achievement, students face unaddressed emotional strain. Institutions should embed mental health support into curricula, create safe disclosure environments and policies, train faculty in emotional literacy to raise resilient, well-supported healthcare professionals.